Malosio Maria Luisa
 Senior research scientist
Senior research scientist
URT c/o Humanitas Research Hospital
Via Manzoni 56
20089 Rozzano
Questo indirizzo email è protetto dagli spambots. È necessario abilitare JavaScript per vederlo.
Maria Luisa Malosio is a cellular and molecular biologist who has developed over the years a strong interest in translational research. To her background belong experiences in neuropharmacology, molecular and cellular biology of topics related to neurosciences, neurosecretion and diabetes.
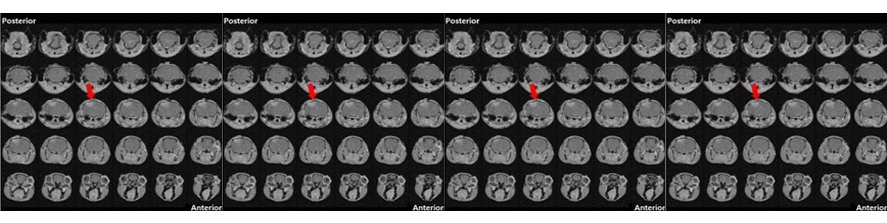
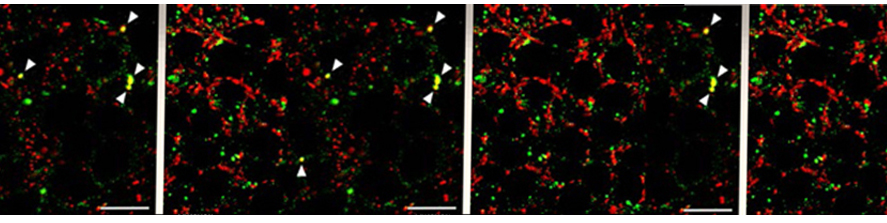
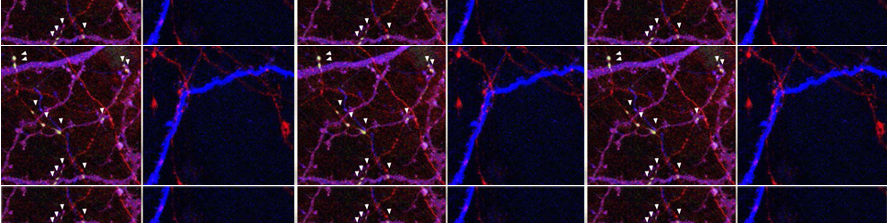
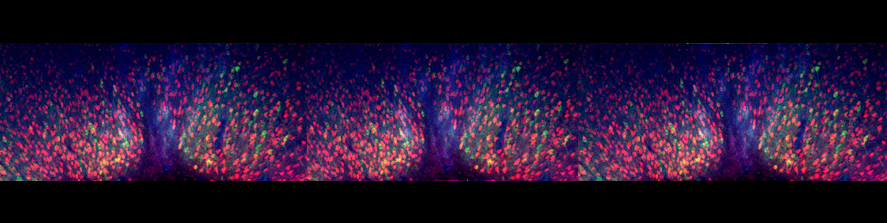
Born in Milano, Italy, where she obtained her Master in Science, she then continued her training at the ZMBH Institute of the University of Heidelberg (Germany), where she got a PhD in Life Sciences. Back in Italy she first worked at the Medical Pharmacology Institute obtaining a Research Doctorate in Pharmacology, then as a post-doctoral fellow at the San Raffaele Scientific Institute. Afterwards she was visiting scientist at the Glaxo-Wellcome Medicines Research Center (UK). Back to the San Raffaele Scientific Institute she worked as a Telethon post-doctoral grantee contributing to the elucidation of the molecular and cellular mechanisms governing neurosecretory granules formation. Later she became project leader within the San Raffaele Diabetes Research Institute developing an interest for non-invasive imaging applied to pancreatic islets transplantation in animal models and patients and in aptamers as novel tools for molecular imaging and targeting of beta cells. Since 2011 she is staff scientist at the CNR.
Member in Academic Societies
ABCD (Associazione di Biologia Cellulare e del Differenziamento) since 2013;
ESOT (European Society of Organ Transplantation) since 2010; SID (Società Italiana Diabetologia) since 2009; ESMI (European Society for Molecular Imaging) since 2009; EASD (European Association for the Study of Diabetes), since 2007; Transplant Society, 2007-2010; ASCB (American Society for Cell Biology) 1996-2001; Heidelberg Alumni International since 1997; Heidelberg Alumni University Ambassador since 2013.
http://www.linkedin.com/pub/maria-luisa-malosio/11/3b/5b3
ORCID 0000-0003-0626-3066